Effective EHR Integration Strategies to Maximize EHR Efficiency
- Updated: Mar 18, 2026
- 10 min
The EHR startup scene is evolving, with new companies penetrating the market. It is no wonder that Electronic Health Record systems have become the central resource for provider workflows. These electronic software solutions facilitate administrative and clinical activities for healthcare organizations.
According to The Office of the National Coordinator for Health Information Technology (ONC), 78% of office-based physicians and 96% of non-federal acute care hospitals adopted a certified EHR in 2021.
EHR integration allows healthcare providers to make informed clinical decisions based on a complete, up-to-date patient medical record. It can streamline the associated administrative and revenue cycle tasks of patient care.
Integrating EHRs across the healthcare operation has numerous benefits. However, this is quite a complex process, with many pitfalls along the way we came across when providing EHR software development services. Here, we will explore the following aspects of EHR integration:
- How EHR integration works
- Benefits of EHR integration
- Challenges of EHR integration
- Strategies for effective electronic health record integration
- EHR integration costs
- Role of EHR integration in clinical decision-making
Let’s explore them all.
Empower your practice with custom EHR/EMR solutions tailored just for you.
How EHR Integration Works
EHR integration links separate systems through interoperability solutions like APIs and standardized protocols. For example, when a laboratory updates test results in its system, the sensitive patient data is automatically reflected in the patient’s EHR. This ensures all healthcare providers have access to the latest information in real-time.
Integration can also include external solutions like prescription monitoring programs or clinical decision support systems, which enhance the functionality of EHR platforms.
The University of Vermont Medical Center successfully integrated its EHR systems using Epic Systems. This allowed for a unified health record accessible across all facilities, improving efficiency, care coordination, and data accuracy despite challenges like interface monitoring and staff training.
Here is a detailed breakdown of EHR integration, including the timelines for each stage: 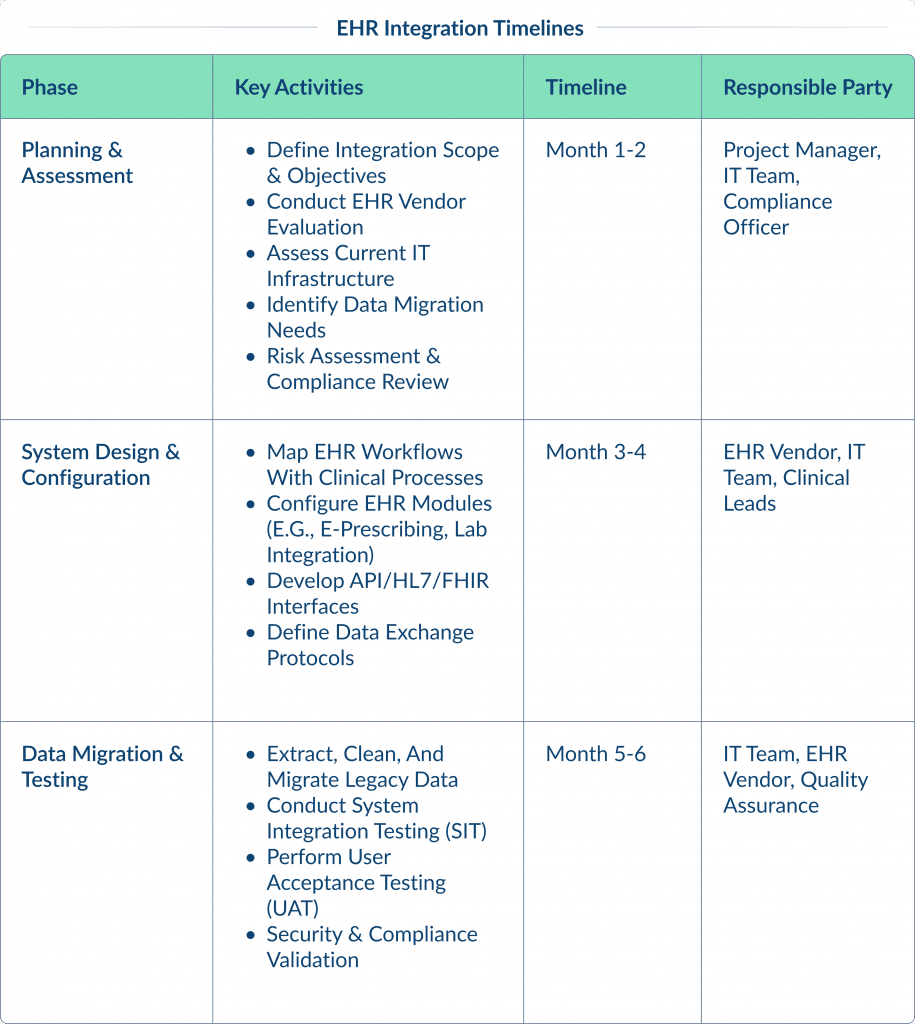
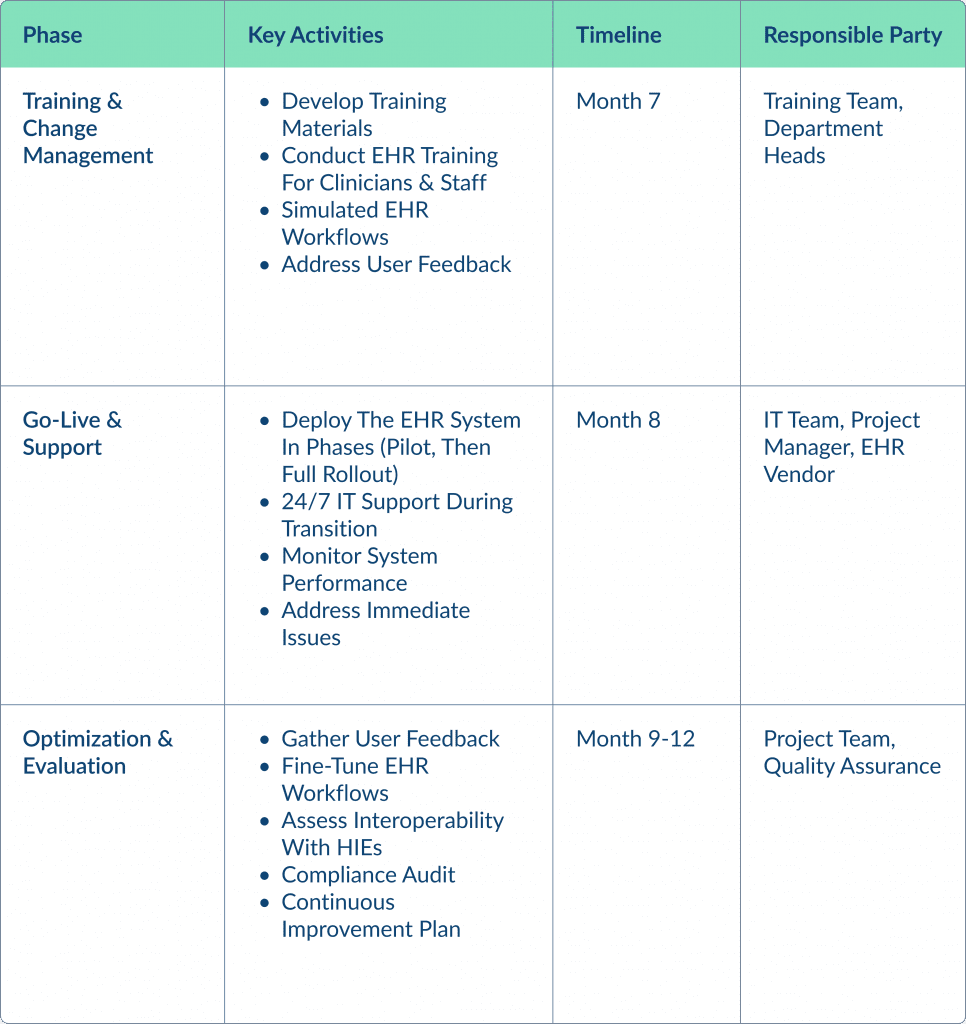
Benefits of EHR Integration
Here are the main benefits of EHR integration, highlighted by ASTP records:
Improved Patient Outcomes
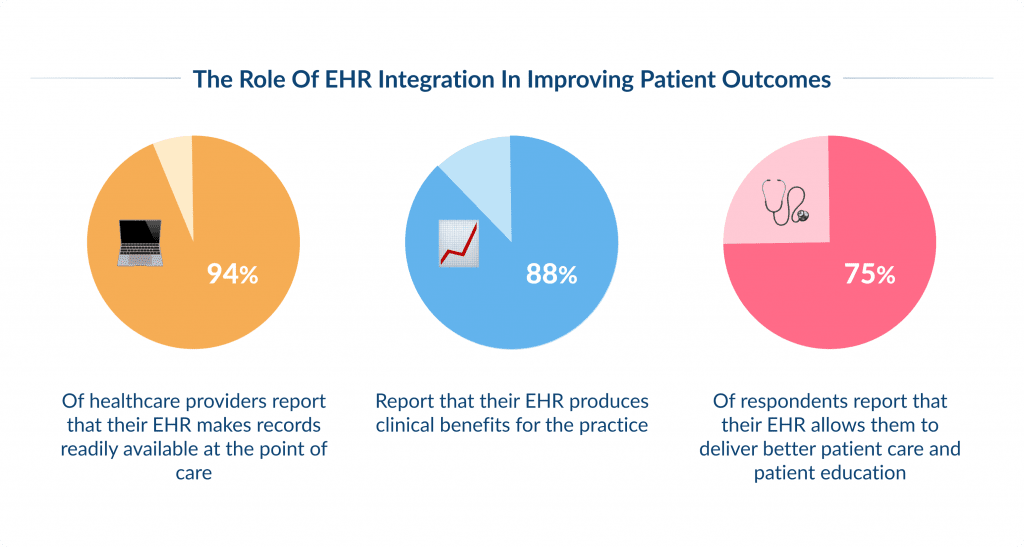
Patients receive better medical care because healthcare providers are better equipped with accurate patient information. Electronic health records can improve the ability to diagnose diseases and reduce, even prevent, medical errors. This leads to better patient satisfaction. The US national survey of doctors showcases that:
- 94% of healthcare providers report that their chosen EHR system makes records readily available at the point of care.
- 88% report that their EHR produces clinical benefits for the practice.
- 75% of respondents report that their EHR allows them to deliver better patient care and patient education.
Increased Efficiency
The abovementioned report highlights that EHRs boost organizational efficiency in healthcare and provide a positive return on investment.
Some standard administrative processes that EHRs can help streamline include:
- Appointment scheduling. This feature prevents common mistakes, such as double booking. It offers real-time scheduling updates that allow providers to reschedule appointments or send patient reminders. Here is more about the doctor appointment app development process, if you are interested to learn more about this topic.
- Billing. An EHR system can reduce the chances of missed or delayed payments as the system automatically generates and sends bills to patients and identifies discrepancies such as duplicate charges or incorrect billing codes.
- Patient communication. Besides providing access to patients’ personal health information much more quickly, EHRs offer messaging platforms that allow patients to ask their providers questions through a secure and confidential method.
These improvements can help healthcare providers manage their workload efficiently. They also prevent human errors, such as indecipherable handwriting or misplaced paperwork. 
Enhanced Accuracy
To provide a well-rounded treatment, doctors need to have access to relevant patient information, such as allergies, chronic diseases, and current medications. This helps them avoid giving patients drugs that could be dangerous or could cause problems with other medications the patient is already taking. It also ensures that patients are safe and that doctors have the information they need to make proper recommendations.
EHR systems prevent medication errors by alerting healthcare providers to potential problems and making it easier to prescribe medications. These systems can save money in the healthcare sector, which spends about $20 billion each year due to medical mistakes.
Regulatory Compliance
EHR system integration is key to compliance. It helps with HIPAA compliance through patient data encryption, implementing access controls, and maintaining audit logs. HL7/FHIR standards integration allows for data analysis and exchange while being compliant with interoperability rules like CMS Promoting Interoperability.
Automated documentation in EHRs reduces errors and helps with MACRA/MIPS and Meaningful Use reporting. Real-time reporting helps organizations comply with state and federal regulations and avoid penalties and patient harm.
If you are exploring opportunities for HIPAA-compliant app development, check out our recent guide. 
Cost Reduction
The cost-savings benefit of EHRs for healthcare systems is debated since different EHR systems are fairly expensive to maintain. However, several aspects of EHR systems save money long-term.
For example, EHR systems reduce the need for paper-based systems, decrease time spent on administrative tasks, and minimize medical errors and inefficiencies.
Common EHR Integration Challenges
Regardless of a healthcare organization’s EHR system, integration with external systems remains a major headache. Clinicians are already struggling with the day-to-day EHR experience, and interoperability just adds another layer of frustration.
In fact, according to the Net EHR Experience Survey (NEES), external integration is the lowest-rated metric out of 11. Only 44% of clinicians say their EHR meets expectations when it comes to connecting with outside organizations. That’s a big problem in a healthcare landscape that increasingly depends on seamless data sharing.
In this chapter, we’ll unpack the key challenges behind EHR integration.
Interoperability
Physicians most frequently cite interoperability as a challenge and report that it is their top fix request. They note that external patient data often isn’t readily available in their EHR and, if found, is difficult to leverage. 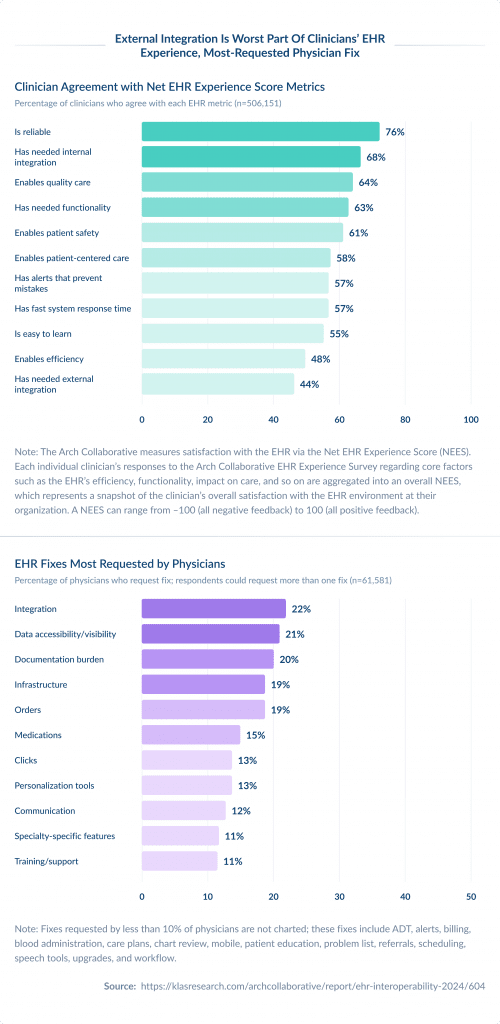
Vendor lock-in feature, as in Epic’s proprietary ecosystem, discourages data sharing with competing EHR technologies. Some healthcare organizations resist sharing data due to competitive concerns or fears of healthcare data breaches.
Additionally, regional differences in interoperability adoption (e.g., some HIEs use FHIR, others rely on older HL7 standards) make it harder to achieve seamless communication between systems. Especially when patients receive care across multiple regions or networks using different standards.
Lack of Standardization
The Arch Collaborative asked over 33,000 clinicians about their experience using outside patient data. Many emphasized that data from outside sources is often challenging to find.
Almost half of respondents report they can’t quickly find critical patient health status information from outside organizations, and another 47% say they have to sift through duplicated data.
“The EHR allows us to pull in information for some patients, but there are times when the information is not accurate. EHRs can interpret information for things like immunizations differently, so if we are not careful, we can incorrectly document that a patient has received a vaccine.” — Nurse
“There are too many places for outside records to be found. I spend a lot of time looking for records.” — Physician 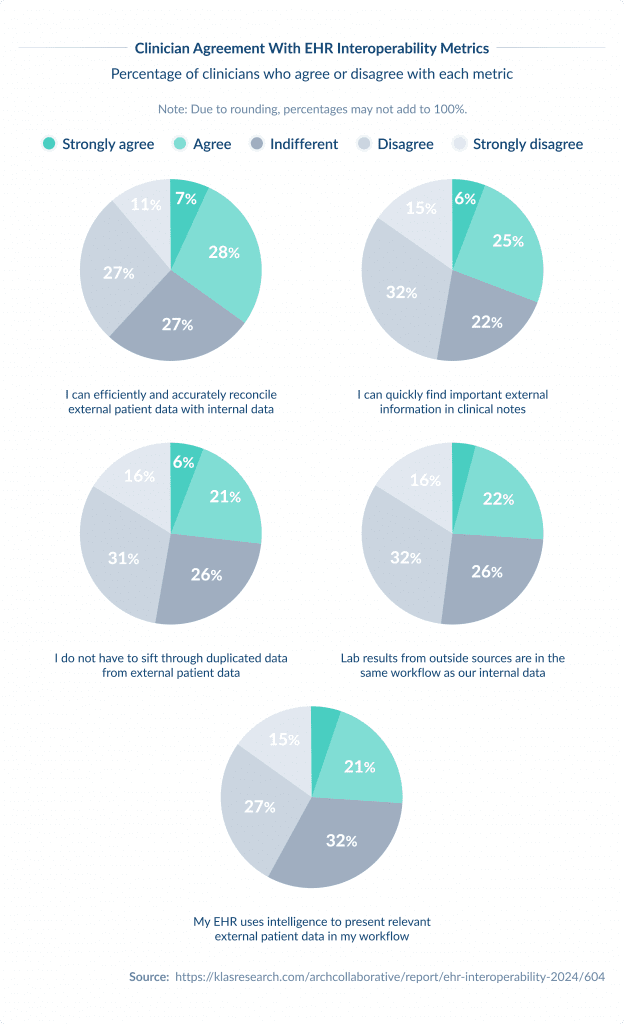
Data Migration Issues
Legacy EHRs often store data in outdated or inconsistent formats. This makes data extraction and mapping difficult. Missing or incomplete fields, such as unstructured clinical notes, require manual cleanup before migration.
On top of that, poor data quality (duplicate records, outdated entries) increases the risk of errors in the new system. This results in data loss or corruption during migration, compromising patient safety.
Clinicians may distrust the new system if patient records are incomplete or inaccurate.
Regulatory Compliance
EHR integrations must support secure data exchange through features like encryption, audit logs, and role-based access controls to protect patient information and meet legal requirements.
When integrating third-party tools, such as telemedicine applications, diagnostic labs, or billing systems, organizations must make sure these vendors also meet compliance standards like HIPAA or CMS regulations.
The regulatory landscape is constantly evolving. For example, CMS interoperability rules require systems to provide patient access to their data and support data sharing across platforms. This means healthcare organizations must regularly update their systems to stay compliant and provide all the necessary data security measures.
Failure to comply can lead to hefty fines, legal consequences, or data breaches. For smaller clinics, keeping up with the technical and financial demands of compliance can be especially challenging.
High Implementation Costs
EHR licensing fees require a considerable investment. For example, Epic EHR can cost $1.5M+ for a mid-sized hospital. Customization, training, and IT infrastructure upgrades add to expenses.
To save money, smaller practices may cut corners. However, this may lead to poor integration or usability issues.
Budget constraints delay or limit integration capabilities. Since ROI is slow, it can frustrate stakeholders who expect immediate workflow improvements.
When EHR systems and practice management software aren’t integrated effectively from the start, it often leads to additional costs down the line. It can occur through manual workarounds, inefficient billing, or the necessity of third-party fixes.
Staff Resistance and Training Challenges
Clinicians often worry that new EHR systems will disrupt their workflows and add more documentation. Without proper training, many end up making errors, relying on workarounds, or avoiding the system altogether.
According to the KLAS Arch Collaborative, primary care physicians report the lowest satisfaction with EHRs. It’s about 22 points lower than other clinicians. This gap in adoption not only affects care quality but also contributes to higher rates of burnout.
Technical Problems
Technical issues like downtime during go-live, system crashes, slow performance, or compatibility issues frustrate users and disrupt patient engagement and care.
Poor healthcare app design, with clunky interfaces, excessive clicks, only worsens the dissatisfaction with the system. This results in lost productivity and delayed care due to technical failures.
That can push healthcare professionals back to manual processes, undermining the multiple EHR system benefits. 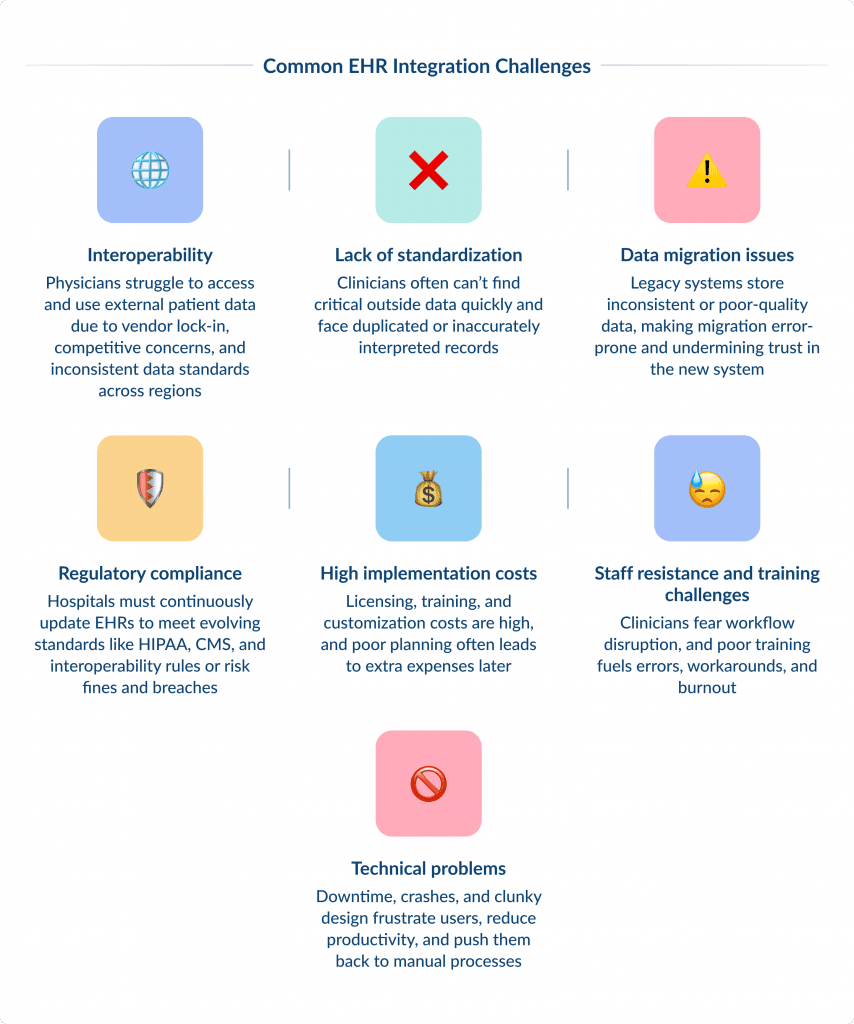
Strategies for Effective Electronic Health Record Integration
Successful EHR integration requires careful planning, collaboration, and adherence to best practices to overcome the challenges mentioned above. Some of the key strategies for effective EHR integration include the following steps:
Adopt Standardized Protocols
Major EHR vendors like Epic and Cerner use widely accepted standards like HL7 (Health Level Seven) and FHIR (Fast Healthcare Interoperability Resources) to share patient data with external apps (e.g., Apple Health pulls records via FHIR). Cerner and Epic have much in common, so check out how they differ in our Cerner vs Epic guide.
Another standard, DICOM, is vital for integrating imaging data (like X-rays or MRIs) with the patient’s EHR. A radiology department, for instance, can instantly upload and view imaging data through the EHR without switching systems. Here is more about how radiology information systems work and integrate with other systems.
Develop a Comprehensive Implementation Plan
Formulate a detailed strategy that includes milestones, roles, and responsibilities for team members. For example, assign data engineers to migrate legacy system data securely while minimizing operational disruptions.
A phased rollout, such as integrating lab systems first, followed by billing, allows teams to test each component in real time, identify problems early, and reduce system-wide downtime.
Here is an example of an implementation plan: 
Leverage APIs
APIs allow EHRs to “talk” to other systems securely and efficiently.
Healthcare organizations rely on API integration and development services to connect their EHRs with medical practice management software, pharmacy platforms, or even third-party billing systems in real-time.
For example, a clinic might use an API to automatically sync appointment schedules between their EHR and telehealth platform to eliminate double entries and manual updates.
Optimize Data Migration
Moving data from an old system to a new one is often a pain point. But proper preparation makes all the difference.
Start with a data audit: identify what needs to be migrated, clean duplicate records, and standardize formats.
Use migration tools that automate the extraction, transformation, and loading (ETL) of historical data. For example, you can use scripts to convert legacy codes to standardized SNOMED CT or LOINC codes, which improves clinical accuracy and system compatibility.
The goal is to move clean, usable data, not just transfer everything and hope it works.
Train Staff and Facilitate Adoption
Even the best integrated system won’t help if people don’t know how to use it.
Offer tailored training sessions for different roles: clinicians, front-desk staff, billing personnel, and IT teams.
Bring in “super users” early in the process, trusted internal specialists who can test the system and give real-time feedback to improve usability.
Invest in Interoperability Solutions
Participating in Health Information Exchanges (HIEs) allows organizations to share patient data securely across providers and regions. A hospital ER can access a patient’s medical history from an out-of-state clinic via an HIE. For example, if a patient is visiting an ER while traveling, doctors can quickly access their medical history (allergies, medications, prior diagnoses) through the HIE. This improves safety and treatment decisions.
In some cases, replacing outdated systems with a unified EHR platform can save time and money long-term. For example, a group practice might switch from multiple disconnected tools to an all-in-one solution like Athenahealth or eClinicalWorks.
Implement Security Measures
Use encryption, access controls, and regular audits to safeguard patient data.
Ensure full HIPAA compliance during integration, especially when transferring sensitive health records or connecting to external systems.
For example, role-based access can ensure that only authorized personnel can view sensitive behavioral health notes within a broader EHR.
Monitor and Optimize Workflows
The job isn’t over after going live. Gather user feedback regularly to identify friction points. For example, the referral process may be slower now, or clinicians struggle to easily locate lab results.
Use healthcare data analytics tools to monitor system usage, task completion times, and user behavior.
These insights help IT teams make data-driven tweaks that continuously improve clinical workflow efficiency and patient satisfaction. 
EHR Integration Cost
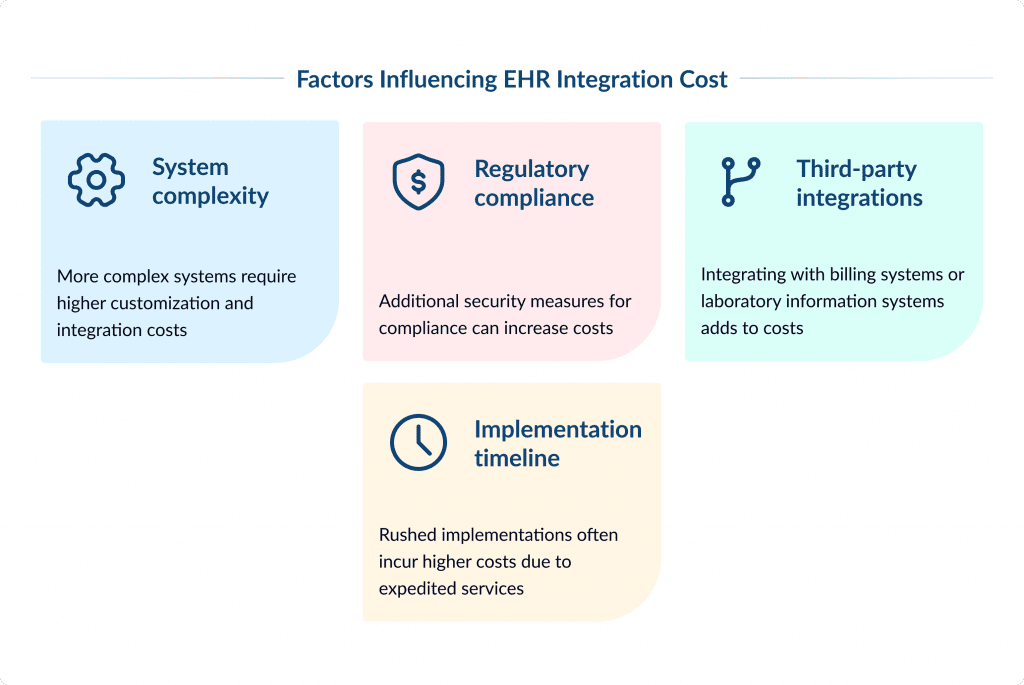
Just like EHR software development, the cost of integrating EHR systems can vary widely based on several factors. These include:
- System complexity: more complex systems require higher customization and integration costs.
- Regulatory compliance: additional security measures for compliance can increase costs.
- Third-party integrations: integrating with billing systems or laboratory information systems adds to costs.
- Implementation timeline: rushed implementations often incur higher costs due to expedited services.
Total Estimated EHR Integration Cost depending on the size of the healthcare organization:

EHR Integration Cost Breakdown (Example)
This is an example of EHR software integration costs. The final cost can vary greatly depending on the factors described above: 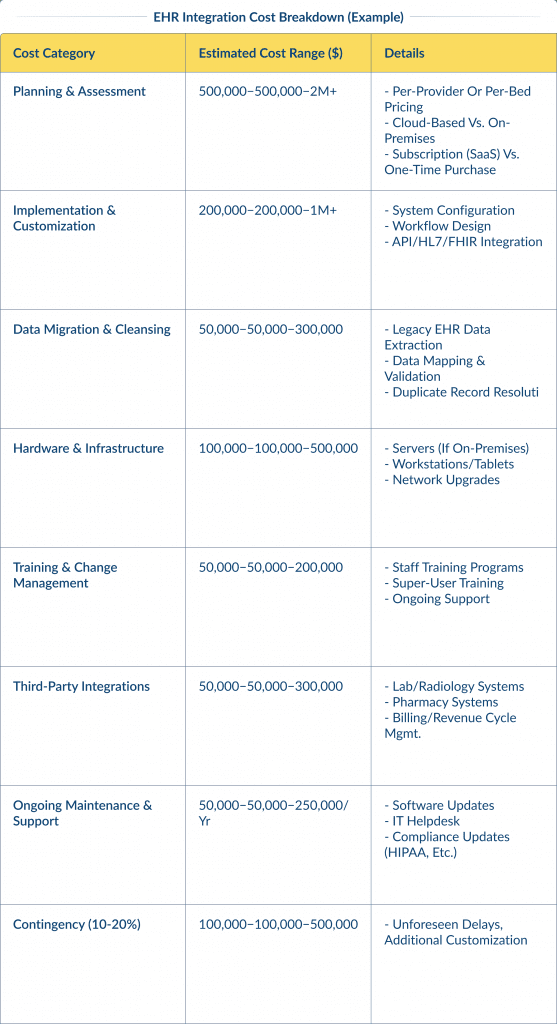
Wrapping up: Role of EHR Integration in Clinical Decision-Making
Electronic health record (EHR) integration helps medical professionals leverage population health insights. These insights are used to improve clinical decision-making and patient management.
New technologies like AI in healthcare, machine learning, blockchain, and telemedicine will further enhance EHR integration. Those technologies will give smarter decision support tools, secure data sharing, and access during virtual consultations.
After all, EHR integration changes clinical decision making and enables medical records to be diagnosed faster, reduces human error, supports personalized care plans, and improves operational efficiency and a more connected healthcare system.
Looking for a healthcare software development partner with a proven track record in telemedicine, patient portal, and EHR software development and design? Contact us for a free consultation to learn more about our approaches and costs.