Predictive Analytics in Healthcare Explained
- Updated: Mar 18, 2026
- 10 min
Healthcare is full of data, but data alone doesn’t save lives. What really makes a difference is being able to spot risks before they become problems. That’s what predictive analytics for healthcare does. It looks at medical records, test results, and even data from wearables to forecast patient health outcomes and guide interventions.
Hospitals and clinics use data analytics tools to personalise their treatment plans and resource allocation. Patients get care that’s proactive, not reactive.
As an EHR and EMR software development company, we help turn complex data into smart solutions that improve patient outcomes and operational efficiency. In this article, we’ll explain what predictive analytics in healthcare is, how it works, and best practices for implementing it.
Get a strategic MVP to mitigate risks.
What is Predictive Analytics in Healthcare?
Predictive analytics in healthcare is about using data mining and smart computer tools to look ahead and forecast what might happen with a patient’s health. Instead of only reacting when someone gets sick, healthcare data analytics helps doctors and hospitals step in earlier, prevent problems, and make better decisions.
At its core, predictive analytics means building models that can answer questions like:
- Is this patient at risk of developing a disease?
- How will their condition likely progress?
- Will they respond well to a certain treatment?
- Are they at risk of being readmitted to the hospital?
This shift, from reacting after something happens to predicting and preventing it, leads to more personalized care and better use of healthcare resources.
How It Works
To make these predictions, predictive analytics uses huge amounts of data and advanced technologies:
- Health data from records, devices, and lab results is collected and cleaned.
- Predictive algorithms and machine learning look for patterns that humans might miss.
- Models are built and tested to see how well they predict outcomes.
Common methods include regression (for risk prediction), decision trees, neural networks, and deep learning, especially for complex data like medical images or genetic information.
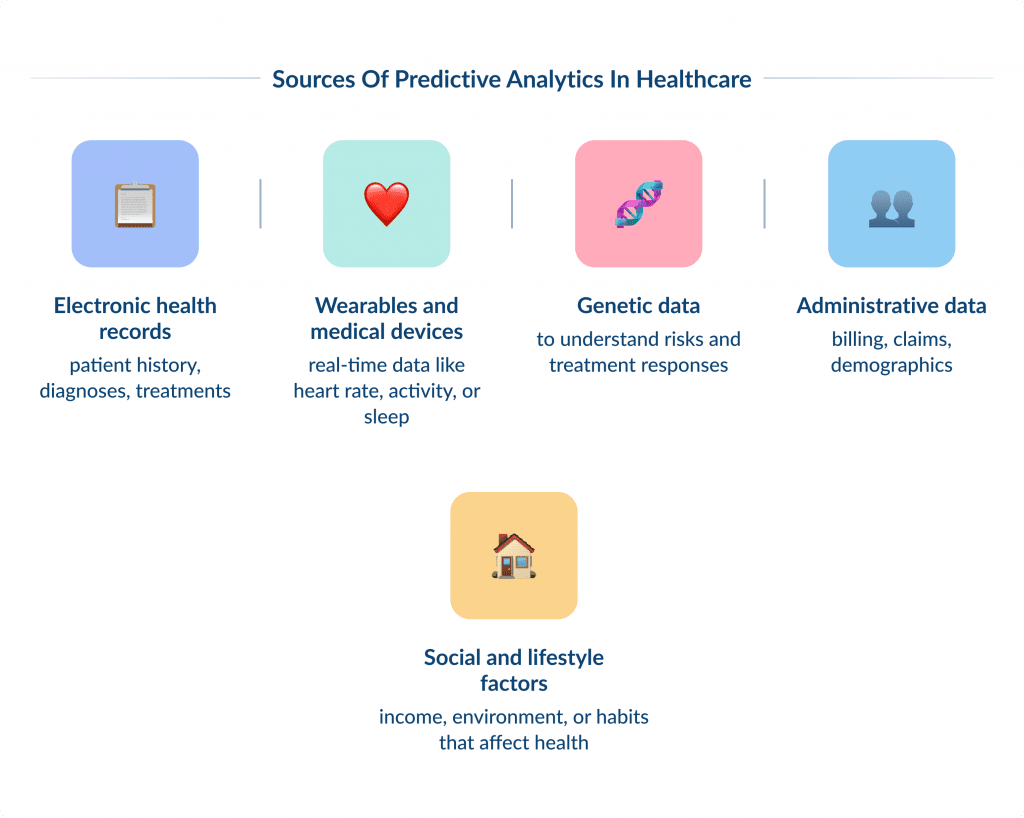
Predictive analytics pulls information from many sources, such as:
- Electronic Health Records (EHRs): patient history, diagnoses, treatments.
- Wearables and medical devices: real-time data like heart rate, activity, or sleep.
- Genetic data: to understand risks and treatment responses.
- Administrative data: billing, claims, demographics.
- Social and lifestyle factors: income, environment, or habits that affect health.
Predictive Analytics in Healthcare: Market Overview
The healthcare predictive analytics market is experiencing significant growth and innovation. In 2025, the market has reached $22.49 billion. It is expected to continue growing at a compound annual growth rate (CAGR) of 24% from 2024 to 2030. This growth is fueled by advancements in technology and evolving healthcare needs. 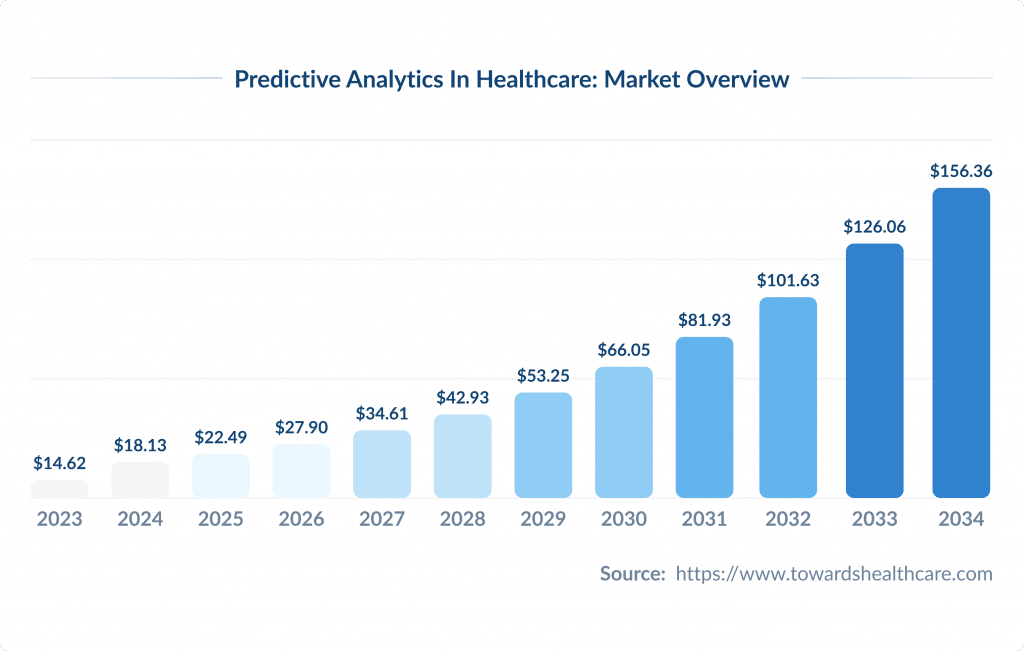
Some other key market trends and drivers include:
- Advancements in AI and Machine Learning (ML)
These technologies are fundamental (here we speak more about AI in product development). They enhance the analysis of complex, large-scale datasets and improve drug discovery, as well as personalized medicine and patient care.
- Increasing volume of healthcare data
The proliferation of electronic health records (EHRs), wearable devices, and mobile health applications generates vast amounts of data, creating significant opportunities for advanced analytics solutions.
- Shift towards personalized and value-based care
Healthcare providers are increasingly focusing on personalized medicine to reduce risks and improve patient care. There is also a rising demand for value-based care, emphasizing tools that can effectively measure outcomes and reduce healthcare costs.
- Chronic disease management
The increasing prevalence of chronic diseases fuels the demand for AI-powered predictive analytics to identify at-risk patients and provide cost-effective treatment solutions.
- Strategic activities and new product launches
New products and partnerships are continuously emerging, such as mPulse launching an integrated predictive analytics product in May 2024, ABOUT Healthcare acquiring Edgility in April 2024 to offer patient progression solutions, and Innovaccer launching a Government Health AI Data and Analytics Platform (GHAAP) in August 2024.
- Preventive healthcare
Predictive analytics serves as a catalyst for preventive healthcare practices, identifying individuals at risk of chronic conditions or adverse health events and enabling targeted interventions.
Benefits of Predictive Analytics in Healthcare
Here are some of the key benefits of predictive analytics in healthcare:
Personalized Care
Predictive analytics models help to create treatment plans that are unique to each patient. It considers the patient’s specific genetic profile, their daily lifestyle, and their complete medical history. This highly tailored approach leads to more effective treatments and greater patient satisfaction because the care feels designed just for them.
Operational Efficiency
Hospitals use predictive models to forecast how many patients will arrive each day. This allows them to smartly allocate resources like beds, equipment, and staff in advance.
These data-driven decisions streamline workflows, cut down on wasteful spending, and ensure the facility runs smoothly for everyone.
Preventive Healthcare
This technology identifies people who are at high risk for developing chronic conditions. Doctors can then intervene early with targeted wellness programs and proactive counseling.
This approach helps prevent illness before it starts, keeping healthier people out of the hospital and improving long-term well-being.
Early Disease Detection
Algorithms can spot subtle patterns and biomarkers that signal the start of a serious condition. They often detect early signs of diseases like cancer or sepsis faster and with more accuracy than traditional methods.
This critical head start allows doctors to begin treatment at the most effective time, greatly improving your chances of a full recovery.
Hospital Readmission Prevention
Predictive tools analyze patient data to determine who is most likely to be readmitted after discharge. Care teams use this insight to provide these individuals with intensive follow-up care and support.
This vigilant, tailored attention helps patients recover fully at home and avoids the stress and cost of returning to the hospital. 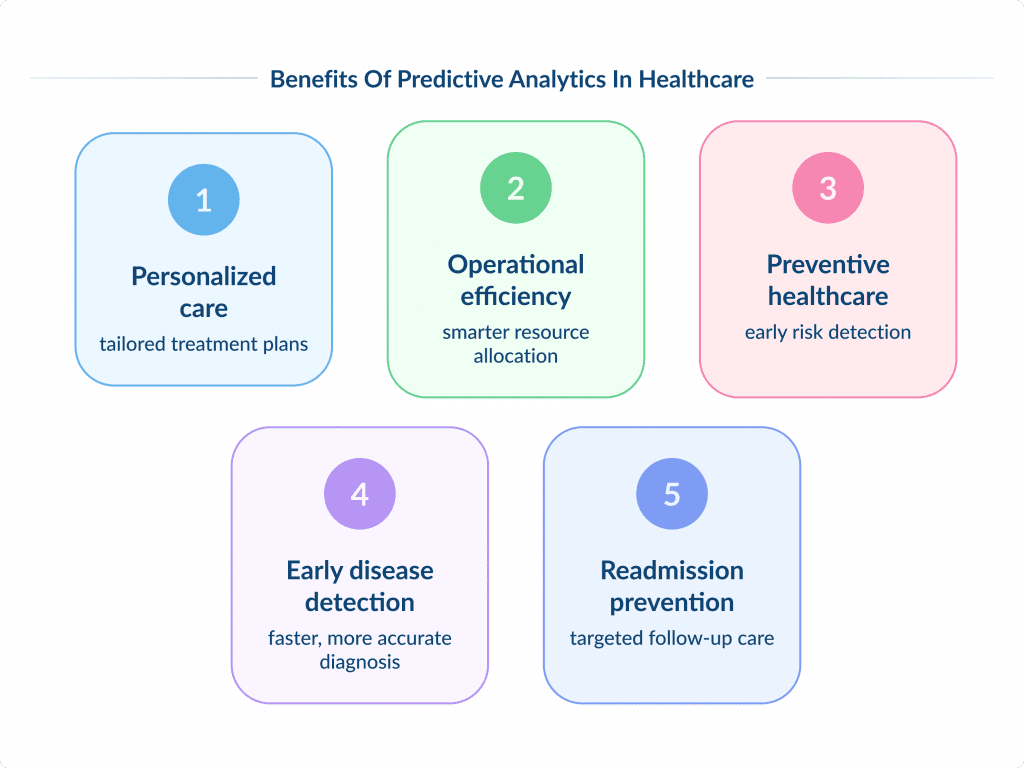
Real-World Use Cases of Predictive Analytics in Healthcare
Predictive analytics is being used in the healthcare industry to tackle many challenges. The main one is to move from reactive to proactive healthcare and improve patient care.
Here are some predictive analytics in healthcare examples:
Preventing Hospital Readmissions and Post-Discharge Care
Kaiser Permanente Northern California (KPNC) implemented the Transitions Program, which used a predictive model to target a care coordination intervention for patients after hospital discharge. This program resulted in a 30% reduction in 30-day non-elective readmissions. The predictive model, called the transition support level score, used 5 variables including lab-based acuity, comorbidity scores, and length of stay.
Another example is Corewell Health, which leveraged AI and predictive analytics to identify patients at high risk of readmission. Predictive healthcare analytics tools helped them prevent 200 readmissions and achieve cost savings of $5 million.
UnityPoint Health, in its turn, built a predictive model to assess patient readmission risk. Using this model helped to reduce readmission rates by 40% within 18 months by enabling early symptom treatment.
Early Disease Detection and Risk Identification
When it comes to disease detection and identifying health risks, predictive analytics is a powerful weapon.
The Targeted Real-time Early Warning System (TREWS) is a machine learning model that was developed and deployed to predict sepsis in hospitalized patients up to 12 hours before traditional clinical detection methods. The goal was to improve the time to treatment and reduce mortality. Johns Hopkins Hospital implemented this model, and it resulted in a 19% reduction in sepsis-related deaths.
Another tool, called the Joslin Risk Stratification Tool (RST), was developed by the Joslin Diabetes Center. Its goal is to identify patients at high risk of diabetes complications.
One more example of using predictive analytics in healthcare is a system implemented by Kaiser Permanente. It uses historical data to identify patients at risk of uncontrolled hypertension and cardiovascular events.
Optimizing Healthcare Operations and Resource Allocation
Healthcare organizations waste billions of dollars due to poor operations and inadequate resource allocation. The American Hospital Association reports that hospitals lose nearly $25 billion each year due to supply chain inefficiencies. This waste is tied to expired inventory, misplaced supplies, and emergency restocking efforts. Predictive analytics can change that.
Children’s Mercy, for example, has launched a Patient Progression Command Center that leverages AI and predictive analytics to optimize care coordination from a patient’s admission through discharge.
Also, ABOUT Healthcare acquired Edgility to provide patient progression solutions with predictive and prescriptive analysis.
Public Health and Disease Outbreak Prediction
Predictive models are aiding in tracking and predicting global health trends, such as the spread of infectious diseases, enabling proactive measures.
For example, BlueDot, a Canadian company, issued a warning about unfamiliar pneumonia cases in Wuhan on December 30, 2019. Nine days before the World Health Organization (WHO) declared the emergence of the novel coronavirus.
Another example is using AI solutions in sub-Saharan Africa to review climate data and local medical reports. The goal is to predict malaria outbreaks.
The UAE Ministry of Health and Prevention (MoHAP) launched a Centre of Excellence for AI in healthcare in October 2023. It is aimed at using big data for predictive analysis in health data digitalization and smart technologies.
Financial Applications and Fraud Detection
The financial application segment, which includes revenue cycle management and fraud detection, dominated the market in 2023, accounting for 35.5% of the revenue. Predictive models help reduce fraudulent claims and manage payments.
Cohere Health introduced early trend signal intelligence in May 2024 to predict medical utilization, enabling health plans to anticipate shifts in medical loss ratios and prepare for potential cost increases.
Another example is when researchers cooperated with Doctor Luis Calvo Mackenna Hospital, a pediatric facility in Chile. They used predictive analytics and ML to reduce appointment no-shows by 10.3% during an eight-week experiment.
These are just a few examples of predictive analytics in healthcare. The implications are numerous and can transform outcomes for patients while saving billions for healthcare organizations.
Challenges and Limitations of Predictive Analytics in Healthcare
Despite numerous benefits, the introduction of predictive analytics in healthcare comes with its challenges and limitations to keep in mind. Here are some of them:
Data Privacy and Security
Healthcare data is highly sensitive, so protecting it from breaches and misuse is critical. Strict rules like HIPAA in the U.S. and GDPR in Europe must be followed at every step.
Algorithmic Bias
If the data used to train models isn’t diverse, the predictions can be unfair, leading to unequal treatment across different patient groups. This is an ongoing concern that requires active monitoring.
Model Explainability and Trust
Many advanced algorithms work like “black boxes” and make it hard for doctors to see why a model made a certain prediction. Without transparency, it’s difficult for clinicians to rely on these tools in critical decisions.
Integration into Clinical Workflows
Even the best models won’t make an impact if they don’t fit naturally into how doctors and nurses work. Seamless integration with existing electronic health record systems and easy-to-use interfaces are key.
Lack of Technical Expertise and High Costs
The development, deployment, and maintenance of predictive tools require specialized knowledge and significant investment. Many healthcare providers don’t have the resources in-house to manage this effectively.
Regulatory and Legal Concerns
Laws around privacy and accountability are complex. It’s still not always clear who is responsible if a prediction leads to patient harm, which creates hesitation around adoption.
Accuracy Trade-offs with Privacy
New privacy-protecting techniques in machine learning are valuable, but they often reduce accuracy by a few percentage points. This trade-off is an important consideration when deploying models in real-world care. 
Best Practices for Implementing Predictive Analytics in Healthcare
Putting predictive analytics into action in healthcare isn’t just about using fancy algorithms and historical healthcare data. It takes careful planning, the right data, and ongoing checks to make sure the tools truly improve patient care and efficiency without creating new risks.
Here are the main best practices:
1. Use High-Quality, Comprehensive Data
- Digitize records. Electronic Health Records (EHRs) are the foundation since they hold patient histories, diagnoses, and treatments.
- Pull from many sources. Add lab results, scans, genetic data, wearables, and lifestyle information to get the full picture.
- Clean and prepare data. Raw data is messy. It must be standardized and organized to work well in models.
- Ensure compatibility. Different hospital systems don’t always “talk” to each other, so standardization and interoperability are key.
2. Build and Test Models Properly
- Pick the right method. Simple regression may work for readmission risk, while complex cases may need advanced machine learning or deep learning.
- Validate carefully. Test predictive analytics solutions on new data to avoid overfitting.
- Measure performance. Use metrics like accuracy, precision, recall, or AUC-ROC to judge reliability.
- Think about impact, not just risk. Focus on patients most likely to benefit from an intervention, not just those at highest risk.
3. Address Ethics and Regulations
- Protect privacy: Follow laws like HIPAA (U.S.) and GDPR (Europe), and anonymize data.
- Reduce bias: Make sure data represents all populations fairly and check models for unintended bias.
- Be transparent. Healthcare professionals need to understand how predictions are made, not just get a “black box” answer.
- Get patient consent. Patients should know how their data is used.
- Define responsibility. Clarify who is accountable if a model’s prediction leads to harm.
4. Fit Into Clinical Workflows
- Keep it user-friendly. Interfaces should be simple and easy for doctors to use during daily routines.
- Integrate with EHRs. Models should work smoothly with existing systems.
- Allow customization. Each hospital or clinic may need adjustments for their own workflows.
5. Involve Key Stakeholders
- Engage clinicians. Doctors and nurses should help shape the tools to ensure they’re practical.
- Include patients. Their input ensures models reflect real-world experiences and build trust.
- Set realistic expectations. Remind users that models provide guidance, not absolute answers.
6. Monitor and Improve Continuously
- Track real-world use. Keep checking how models perform in practice.
- Update regularly. Retrain models with new data as health trends, treatments, and patient needs evolve.
- Commit to quality. Build in processes for ongoing improvement.
7. Plan for Costs and the Future
- Invest in people and tech. Strong infrastructure and skilled teams (or external partners) are essential.
- Consider reimbursement. Current payment models may not yet fully cover predictive tools. Planning ahead is key.
- Adopt new tech. Stay up to date with advances like federated learning (AI that protects privacy while using data across organizations).

Summing Up: The Role of Predictive Analytics in Healthcare
When working on a healthcare project, like this user-friendly EHR system design, we focus on three core principles:
- Interoperability. Providing seamless data exchange across health systems.
- Compliance. Meeting strict healthcare regulations like HIPAA.
- User experience. Designing intuitive interfaces for clinicians.
This EHR solution combines telemedicine, e-prescriptions, EHR, lab tests, and home health services into a single, easy-to-use platform.
During our design process, we put accessibility, trust, and flexibility at the heart of the product. Our goal, as a company specializing in EHR software development, was to create a seamless healthcare experience for people of all ages and abilities.
Predictive analytics adds an extra layer of care to EHR systems. It helps doctors spot early warning signs of disease, predict which patients may need follow-up, and place resources where they make the biggest impact. Patients get faster help and more personal treatment. Providers cut waste and avoid costly surprises. When built into EHR systems, predictive analytics turns them from digital records into true partners in proactive care.