Radiology Information System: Key Components and Benefits
- Updated: Jan 05, 2026
- 15 min
Radiology information systems (RIS) act as a bridge between primary doctors and imaging departments. These systems help teams work together and ensure patients get timely diagnoses and treatments.
As more people access radiology services, hospitals need smarter systems to handle the growing demand. In January 2024, for example, Vertex in Healthcare launched VRIS. This is a radiology information system that helps imaging departments reduce delays and speed up report processing. This was a move to make radiology work more smoothly and for patients to get their results faster.
What benefits does RIS bring for radiology departments? Are radiology information systems really effective? Our company specializes in EHR software development services. Here, we explore what RIS is, how it works, its benefits, and future trends.
If you are a healthcare provider looking to streamline radiology workflows, this guide will help you understand why radiology information system software is essential and how the right software can make a real difference.
Start your journey with our expert developers to bring your app idea into reality - contact us today!
What is Radiology Information System & How It Works?
A radiology information system (RIS) is a software suite and database that manages the entire lifecycle of radiological patient data and diagnostic imaging workflows within medical imaging departments.
It’s the operational backbone or central nervous system for radiology departments that manages all administrative and clinical tasks, from order entry to results delivery.
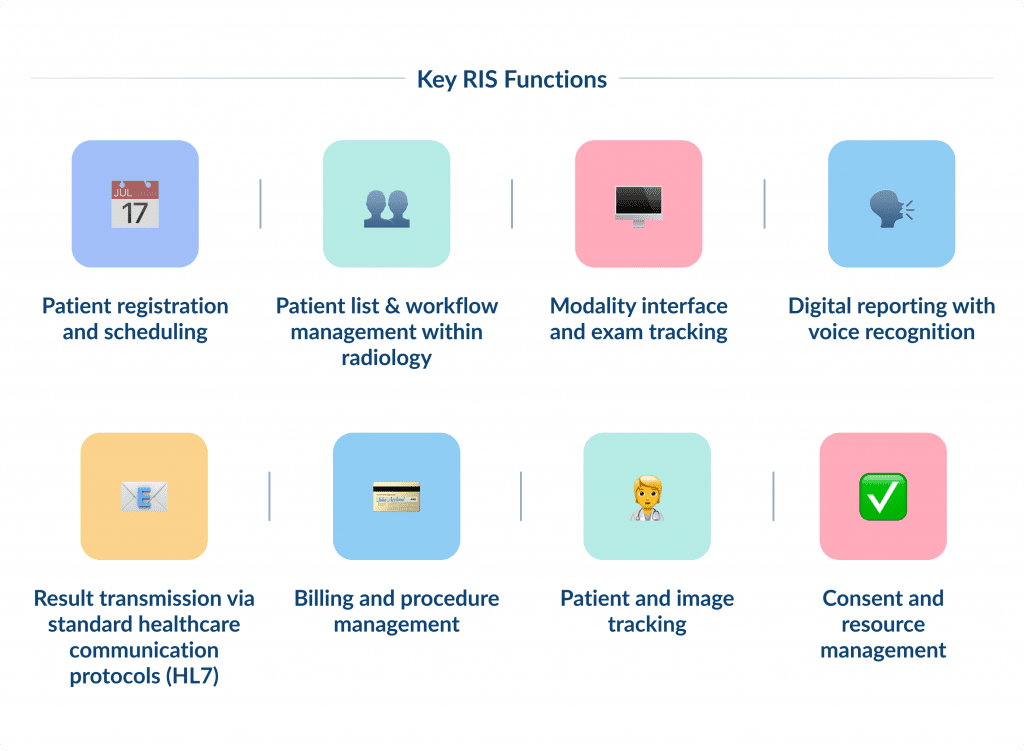
The main goal of an RIS is to simplify operations and ensure communication among healthcare providers. Key functions include:
- Patient registration and scheduling
- Patient list and workflow management within radiology
- Modality interface and exam tracking
- Digital reporting with voice recognition
- Result transmission via standard healthcare communication protocols (HL7)
- Billing and procedure management
- Patient and image tracking
- Consent and resource management
History and Evolution of RISs
RIS has been around for a while, with the first versions appearing in the 80s. At this time, radiology departments were transitioning from manual, paper-based processes to computerized systems.
These early RISs focused on basic patient data management and scheduling appointments more efficiently. They were limited in functions, but they laid the groundwork for digitizing radiology workflow and organizing patient information.
At this point, RIS didn’t have digital imaging, as analog film-based systems were still prevalent. So challenges like cumbersome record storage, difficult retrieval, and human error were still present. Despite these limitations, the first-generation RISs offered better organization and scheduling. This helped to improve operational efficiency in radiology departments.
Later technological advancements, especially the introduction of digital imaging and the development of Picture Archiving and Communication Systems (PACS), made RISs more comprehensive and integrated imaging, reporting, and patient data management.
Now, RIS is an essential part of radiology departments to deliver high-quality patient care.
Key Components of RIS
Radiology information systems are designed to manage the entire lifecycle of radiological patient care data and diagnostic imaging workflows. They coordinate all administrative and clinical tasks, from order entry to results delivery. The key components and functionalities of a modern RIS system include:
Patient Scheduling and Registration
The system takes care of booking imaging appointments, as X-ray, CT, MRI, or ultrasound. It keeps track of available exam rooms and equipment, so nothing overlaps and resources are used effectively.
At the same time, it stores essential details like a patient’s demographics, insurance, and the patient’s complete medical history. To cut down on missed appointments, it also sends out automatic reminders.
Patient Tracking and Workflow Management
From the moment a patient arrives until their examination is finished and the report is ready, the system follows every step of the process.
Radiology staff see clear, prioritized worklists that show who the patient is, what exam they need, and the right imaging protocol to use.
Orders from physicians are managed electronically, while the system also monitors how rooms, equipment, and staff are being used. This helps spot bottlenecks and improve efficiency, which is the essential feature of effective hospital management system.
Radiologist Reporting and Image Tracking
Radiologists get a streamlined list of exams that are ready for them to review.
They can dictate reports using voice recognition and rely on structured templates to make reports complete and consistent.
The system also shows the status of each report: draft, transcribed, or finalized, and connects the report directly to the right images. When paired with PACS, radiologists can move seamlessly from images to reporting in one place.
Results Distribution
Once the reports are finalized, the system ensures they’re securely delivered to the referring physicians. If the hospital uses an electronic health records system, like Cerner or Epic, the results appear directly in the patient’s medical record for quick access.
In urgent cases, the system flags critical findings so they don’t go unnoticed and makes sure the receiving doctor acknowledges them.
Medical Billing and Financial Management
The system gathers all the right details, like procedure and diagnosis codes, so the medical billing is accurate. It can generate claims, connect with billing systems, and track insurance information.
If you want to learn more about healthcare billing, key features, and how it works, check out this guide on medical billing software development.
Inventory and Materials Management
Supplies such as contrast media or catheters are tracked in real time. If stock runs low, the system sends alerts so departments can reorder before shortages happen. This avoids unnecessary delays in patient care.
Business Analytics and Management Reporting
With the help of healthcare data analytics, the system also produces reports that show how many exams are being done, how equipment is being used, and how long patients are waiting. It can track how quickly reports are completed.
These insights help radiology departments improve efficiency, plan for the future, and maintain high standards of patient management. 
Benefits of Radiology Information Systems for Healthcare Providers
RIS keeps the entire radiology process running smoothly. It automates repetitive tasks, centralizes communication, helps to save costs, and more. Here are some key benefits of radiology information systems for healthcare organizations:
Operational Efficiency and Workflow Optimization
The system automates repetitive tasks and centralizes information, which cuts down on errors and saves staff from juggling phone calls and paperwork. A receptionist can instantly see the next available MRI slot and book it in seconds instead of calling around to different departments.
Automated Scheduling and Registration
The system handles appointment scheduling across all imaging types while preventing double bookings. It also stores patient details such as insurance and medical history for future visits.
When a patient needs an MRI, RIS checks room availability, confirms the time, and sends a reminder message so they don’t miss their slot. This leads to fewer delays and shorter waiting lists.
Patient Tracking and Workflow Management
Radiology information system follows every patient step, from arrival through the exam to the final report. Technologists see a clear digital worklist on their console, showing the next exam, patient details, and the correct protocol. This ensures the right patient receives the right procedure without manual data entry or confusion.
Faster Report Turnaround Times
The system speeds up reporting with ready-to-use worklists, voice recognition for quick dictation, and structured templates for consistency. A radiologist can dictate findings straight into the system, finalize the report electronically, and sign it right away. This means the patient’s results are available much faster, reducing the anxious wait between the scan and the diagnosis.
Enhanced Patient Care and Safety
Radiology information systems strengthen diagnostic accuracy, improve safety, and make communication with patients smoother. These improvements directly enhance outcomes and patient satisfaction.
Reduced Diagnostic Errors
Radiologists open a patient’s complete imaging history instantly. Access to past exams supports better comparisons and sharper diagnoses. AI tools highlight unusual areas in images and offer a second perspective. The system also prioritizes urgent cases, moving them to the top of the list for immediate review. A flagged chest CT with suspected critical findings reaches the radiologist without delay, which can change outcomes in emergencies. Standardized reporting templates keep language consistent and results easier to understand for referring physicians.
Improved Patient Safety
Automated processes reduce the risk of human mistakes. The system checks patient identity before exams, verifies that the correct protocol is in use, and issues alerts about allergies or contraindications. Before contrast media administration, RIS warns the technologist if the patient has an iodine allergy or poor kidney function. This check helps staff choose a safer approach without interrupting care. The system also flags critical findings and ensures staff acknowledge them quickly, preventing dangerous delays in urgent treatment.
Enhanced Patient Communication
RIS improves how patients receive and understand information. The system sends reminders ahead of appointments, often with preparation steps included.
If appointment app development is something you are interested in, explore this doctor appointment app development guide for more insights.
A patient scheduled for a CT scan gets a text message with the exact time and prep instructions. The clear guidance reduces stress, prevents missed exams, and helps patients arrive prepared. Patient portals also give individuals access to their results and exam details, keeping them informed and involved in their care journey.
Financial Management and Cost Savings
RIS improves billing accuracy, lowers operating costs, and helps radiology departments handle more exams.
Accurate and Timely Billing
The system records procedure and diagnosis codes automatically and creates clean claims. This reduces denials and speeds up payments. Staff no longer need to re-enter codes after each exam, which shortens the billing cycle.
Reduced Operational Expenses
RIS stores data digitally and eliminates the need for film libraries and paper files. Departments save money on film, chemicals, and storage space. Staff spend less time on manual data entry and more time on patient care.
Increased Throughput and Revenue
Streamlined workflows help exams finish faster and reports reach physicians sooner. Departments can complete more studies in the same time, which raises revenue without extra resources.
Interoperability and Compliance
A radiology information system acts as a central hub for radiology data. It keeps patient information secure and connects smoothly with other healthcare systems.
Seamless Integration with Other Systems
RIS is designed to work in conjunction with Picture Archiving and Communication Systems (PACS), Electronic Health Records (EHRs), and Hospital Information Systems (HIS). A key success factor is a robust EHR integration strategy to reduce manual entry and ensure data consistency across platforms.
Here is how it works. When a radiologist opens images in PACS, RIS displays the patient’s history and prior reports. Once the report is finalized, RIS sends it to the electronic health records system so the referring physician can access it immediately.
Data Security and Regulatory Compliance
Radiology information system protects sensitive data with encryption and strict security measures. It supports compliance with standards such as HIPAA and GDPR. The system records all access and changes, creating a full audit trail. Cloud-based RIS also backs up data to prevent loss if hardware fails. 
Artificial Intelligence in Radiology Information Systems
AI and healthcare are reshaping the future of medicine, making it smarter, faster, and more accessible.
Artificial intelligence and machine learning are increasingly integrated into radiology information systems. This integration is a key trend that is going to shape the future of modern radiology departments. The main goals of introducing AI into RIS are to achieve higher effectiveness and improve healthcare delivery. Here are some more benefits and examples of AI in RIS:
Enhanced Diagnostic Accuracy and Speed
AI algorithms help radiologists spot anomalies and highlight problem areas in images. They act as a second pair of eyes and can even detect issues that are hard to see with the human eye. AI also helps standardize reports, making results clearer and more consistent.
Some systems can analyze images to detect nodules, fractures, or other abnormalities and flag critical findings for urgent review. This reduces the risk of missing important diagnoses.
One such radiology information system example is Aidoc’s AI. This solution has been implemented in multiple medical centers to detect and prioritize incidental pulmonary embolism (iPE) on chest CT scans not specifically intended for pulmonary embolism diagnosis.
In a study of over 14,000 CT scans, the AI correctly identified 84.8% of cases and accurately ruled out 99.1% of non-cases. This shows it can improve workflow and catch serious conditions that might otherwise be missed.
Efficient Workflow
AI organizes worklists and flags urgent exams first, so radiologists focus on the most critical cases. It also helps schedule appointments based on urgency, machine availability, patient history, and predicted no-show rates.
Calantic’s AI system, for example, automatically checks new scans and patient data, flags urgent cases, and sorts studies so radiologists see the most critical ones first. It can also suggest the right imaging protocol and alert staff if something needs immediate attention. This way, doctors have more time to focus on diagnosing instead of managing the workflow.
Automated Reporting
AI assists with drafting preliminary reports and structuring findings. Radiologists review and finalize these reports, saving time on documentation. Natural language processing (NLP) can check dictated reports for completeness, spot errors, and extract data for research or analytics. This speeds up report creation and reduces mistakes.
Advanced Analytics and Decision Support
When integrated in RIS, AI analyzes RIS data to predict patient no-shows, optimize scheduling, or forecast equipment maintenance.
Clinical decision support (CDS) provides relevant patient information and suggests possible diagnoses or imaging strategies. AI-powered dashboards give real-time insights for better operational decisions and smoother workflows.
Data Integration and Infrastructure
AI needs all patient data to be connected and standardized. Formats like HL7 and DICOM make it easier for AI to process images and other clinical information. AI also supports advanced projects like radiomics, which analyzes every parameter in medical images to provide quantitative insights.
Overall, the use of AI in RIS and PACS is moving from research into everyday clinical practice. It helps radiologists work smarter, improves diagnostic accuracy, and makes patient care faster and safer. AI is becoming a central tool in modern radiology. It supports professionals and improves patient care quality worldwide.
Implementing RIS
Implementing a Radiology Information System (RIS) takes careful planning. Hospitals need to make sure it works smoothly with other systems like EHRs (patient records) and PACS (image storage). The system must follow regulations like HIPAA to keep patient data safe. It also has to be easy for staff to use to avoid mistakes. Here is more about HIPAA regulations and HIPAA-compliant app development.
A real example is in South Australia, where all South Australian Medical Imaging sites use Annalise.ai with RIS. This AI reviews chest X-rays, highlights areas of concern, and suggests possible diagnoses. Radiologists still make the final call, but the AI helps them work faster and improves accuracy across multiple hospitals.
Overview of Key RIS Implementation Phases
There are three key phases of implementing RIS. These include:
- Phase 1: Strategy & Planning (The “Why” and “What”)
- Phase 2: Execution & Build (The “How”)
- Phase 3: Launch & Growth (The “Now” and “Next”)
Let’s explore what each phase entails.
Phase 1: Strategy & Planning
This initial phase is about defining goals, building your team, and choosing the right solution.
| Aspect | Key activities | Considerations & best practices |
|---|---|---|
| Defining goals | Identify pain points (manual reporting, siloed data) and desired outcomes (reduced admin burden, improved grant success). | Start with ‘Why’. The project’s purpose must be clear and aligned with the institution’s research strategy. |
| Building the team | Form a cross-functional project team and steering committee. Secure a strong executive sponsor. | A passionate, influential executive sponsor is critical for overcoming obstacles and securing funding. |
| Requirements gathering | Hold workshops with all user groups (researchers, admins, leadership) to gather functional needs. | Involve users early. Faculty and admin staff are the primary users. Their input is non-negotiable for adoption. |
| Vendor selection | Create a Request for Proposal (RFP), demo systems, check references, and evaluate against your needs. | Check integration capability. The RIS must integrate with existing systems (HR, Finance, etc.) via APIs. |
Phase 2: Execution & Build
This phase focuses on configuring the system, managing data, and preparing for launch. If you are a project manager in healthcare, see this guide covering healthcare project management strategies & methodologies.
| Aspect | Key activities | Considerations & best practices |
|---|---|---|
| Project management | Develop a detailed project plan with a timeline, milestones, and assigned resources. | Implement in phases (Profiles first, then Grants) to manage complexity and risk. |
| System configuration | Work with the vendor to set up the system, workflows, and user permissions without excessive customization. | Customize minimally. Heavy customization increases cost and complicates future upgrades. Use out-of-the-box features where possible. |
| Data migration | Identify legacy data to migrate, clean it extensively, and map it to new fields in the RIS. | Data quality is paramount. Dedicate significant time to data cleansing before migration. |
| Integration & testing | Build and rigorously test connections (APIs) to other systems (HR, Finance). Conduct User Acceptance Testing (UAT). | Test real-world scenarios. Have end-users test common tasks like submitting a grant or updating a profile to find gaps. |
Phase 3: Launch & Growth
This phase entails a smooth go-live, promotes adoption, and plans for the future.
| Aspect | Key activities | Considerations & best practices |
|---|---|---|
| Training & support | Develop role-based training (for researchers vs. college admins). Create quick-reference guides and a support plan. | Offer live workshops, video tutorials, documentation, and other blended learning methods to cater to different learning styles. |
| Communication | Communicate the go-live date, benefits, and support channels clearly and repeatedly through multiple avenues. | Be transparent about the transition period and that there will be a learning curve. |
| Go-live & stabilization | Execute the launch plan. Have a dedicated “command center” team ready to answer questions and fix issues immediately. | Provide ample support. Go-live is the beginning, not the end. Expect a high volume of questions in the first few weeks. |
| Continuous improvement | Gather feedback, monitor system usage, and create a roadmap for new features, phases, and optimizations. | Establish a governance model. Create a group to prioritize future enhancements based on user feedback and strategic goals. |
Successful implementation is a complex, strategic project that requires careful planning and cross-institutional collaboration. It is better to work with an experienced implementation partner and a dedicated, cross-functional team from within your institution.
Future Trends in RIS
The global RIS market reached $1.1 billion in 2025, and its importance in the healthcare industry will only grow.
Hospitals and clinics are using RIS more and more, especially after COVID-19 showed the need for strong digital tools. New technologies are making RIS smarter and faster. They help radiology teams handle more exams, reduce delays, and give patients quicker, more accurate results. Here are some key healthcare technology trends that will shape the future of RISs and other imaging data software:
Artificial Intelligence (AI) and Machine Learning
AI integration is transforming RIS by automating processes, enhancing diagnostic accuracy, and improving workflow efficiency. AI helps in image interpretation, anomaly detection, predictive analytics in healthcare for early disease detection, and reducing human error. AI-driven solutions also support voice recognition and natural language processing for faster reporting.
Cloud-Based Systems
More hospitals are moving RIS to the cloud. Cloud systems scale easily and let staff access data from anywhere. They make collaboration and data sharing simpler and speed up workflows.
Using cloud application development services, healthcare providers can create customized RIS solutions that fit their needs. Security is improving, and these systems follow healthcare rules to keep patient information safe. Cloud-based RIS also reduces the need for physical servers and IT maintenance, saving hospitals time and money.
Enhanced Interoperability
According to the recent Mordor Intelligence report, RIS is advancing towards better interoperability with other healthcare systems like electronic health records systems, PACS, and hospital-wide information systems through standards like HL7 and FHIR.
This makes real-time data exchange seamless, reduces redundant data entry, and supports integrated patient care.
Patient-Centered Care and Engagement
Future RIS systems are giving patients more control over their health information. Patients can easily view their imaging reports and history, which helps them stay informed and involved in their care. This approach supports personalized medicine, letting doctors tailor imaging and interpretation to each patient. For example, some hospitals now allow patients to access their X-rays and MRI results through secure patient portals, so they can review their information before appointments and ask informed questions.
Data Security and Cybersecurity
RIS systems manage a growing amount of sensitive patient and imaging data, so strong security is essential. Modern RISs use encryption, audit trails, and other security measures to keep information safe.
They also follow healthcare rules to safeguard patient privacy and maintain trust. Recently, the U.S. Department of Health and Human Services proposed new cybersecurity requirements for healthcare organizations. These include mandatory multifactor authentication, network segmentation, and data encryption to better defend against cyber threats.
All these changes show a future where RIS systems are smarter, safer, more connected, and focused on patients while keeping up with evolving technology and regulations. 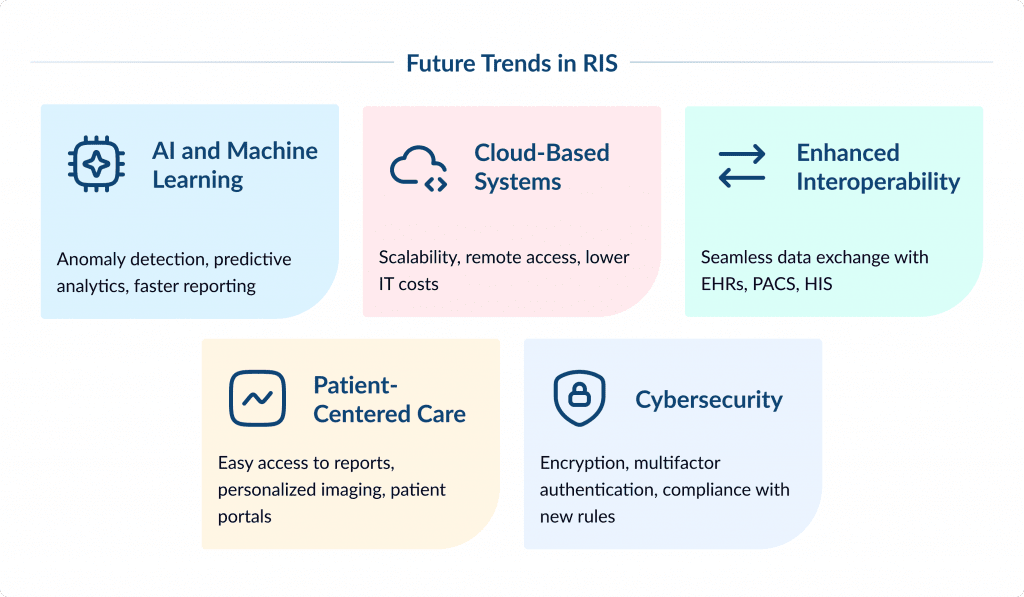
Key Takeaways
Medical imaging is one of the most frequently used diagnostic tools. The volume of CT, MRI, X-ray, and ultrasound scans continues to grow annually due to an aging population and the critical role of imaging in diagnosis. In this context, a modern RIS becomes a core piece of health IT infrastructure, just like an EHR.
Healthcare is shifting from fee-for-service (getting paid per procedure) to value-based care (getting paid for patient outcomes). A RIS helps prove value by:
- tracking efficiency
- reducing duplicate scans
- ensuring proper reporting
- contributing to better patient outcomes.
In fact, modern RIS platforms move beyond simple scheduling and tracking. They become analytical powerhouses, fueled by AI, ML, NLP models, cybersecurity measures, and other advanced technologies.
If you are building for the healthcare sector and looking for a reliable software development partner, contact us. At SpdLoad, we build modern, compliant, and secure healthcare software solutions that scale with your needs and protect patient data.